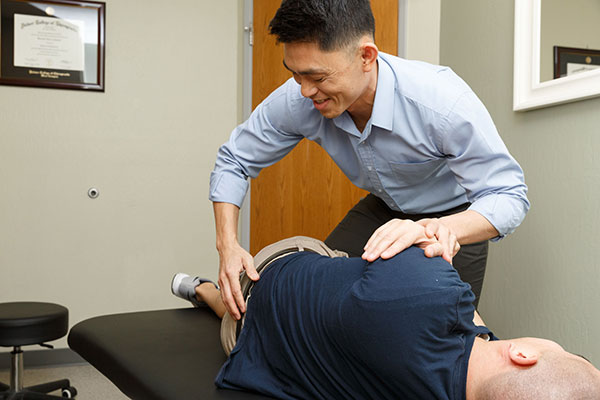
The Chiropractic Approach to Low Back Pain
What is back pain?
Back pain typically occurs in the lumbar spine and pelvic region otherwise known as the buttocks. The pain can occur from a tightening of muscles or joints that get jammed due to a specific incident or small injuries that occur over time from work, athletics or even desk jobs.
What is the most common cause of back pain?
The most common cause of back pain is related to repetitive strain injuries that occur on the job or during daily activities. Working on the computer, cooking, sewing or any activity that keeps you repeating the same movements from the same position can be the culprit of that nagging backache. The strain happens when either the muscles are tight and you are unable to stretch them, or when a joint is misaligned and the muscles become painful as they try to re-align the joint.
What are the less common types of back pain?
Degenerative disc disease, arthritis, herniation and neurologic conditions are all injuries that occur to the spine and more commonly in the low back. These conditions will likely cause you great distress and you will need to seek a health care provider’s services. The following symptoms require an immediate visit to your doctor:
- History of cancer
- Unexplained weight loss >10 kg within 6 months
- Age over 50 years or under 17 years old
- Failure to improve with therapy
- Pain persists for more than 4 to 6 weeks
- Night pain or pain at rest
- Persistent fever (temperature over 100.4 F)
- History of intravenous drug abuse
- Organ transplant
- Recent bacterial infection
- Major muscle weakness
- Trouble lifting your foot
- Numbness and lower extremity weakness
- Anal sphincter dysfunction
- Recent trauma
- History of osteoporosis
What are the basic causes of back pain?
- Desk job
- Osteoarthritis
- Herniated disk
- Gravity
- Sports injury
- Bacterial Infection
- Fractures
- Cancer
- Repetitive strain
- Jammed (misaligned) joints
Why see a Chiropractor instead of a massage therapist?
Chiropractic care helps re-align joints which stops the pain related to the muscles trying to push the joint back into alignment. A typical response to this type of pain might be to stretch or get a massage. While this might temporarily ease the pain, if you don’t re-align the joints, the muscles will loyally return to their job of trying to push the joint back into place and you will be back in pain once again. This isn’t to say that massage can’t be a terrific partner in getting rid of long term pain. We feel that massage and chiropractic can make an excellent team!
Getting adjusted not only will help relieve your low back pain, but offers other health benefits as well. According to research by Sean M. Hannon, BA, DC, chiropractic adjustment can result in the following physiologic changes:
- Increased strength
- Increased oxygen consumption capacity
- Increased range of motion
- Decreased pain
- Increase cardiac regulation
- Increased immunity
Considering these benefits, it is easy to see why athletes and other health conscious people seek out regular chiropractic care. If you suffer from chronic or even occasional back pain, contact our office. We can help!
What are some of the techniques we use to treat low back pain?
Our doctors are trained in many different types of adjustment techniques ranging from hands-on to instrument adjusting. They also use different types of soft tissue therapies that can benefit an injury whether it is chronic or acute. Treating both joint and soft tissue issues allows an injury more complete resolution than either alone. The techniques used are:
- Graston – soft-tissue and fascia therapy
- Activator – instrument adjusting (non-force)
- Sacro-occipital Technique (SOT) – Use of pelvic alignment (non-force)
- Diversified Adjustment – Manual medicine with hands
- Thompson Drop Adjustment – Using the table to increase speed of adjustment but not the pressure put on a body
- Quantum Neurology – instrument adjusting (non-force) uses nerve reflexes as well
- Gonstead – Classic manual chiropractic adjustment
- Kinesio tape – muscle therapy and proprioceptive training using tape
- Cranio-sacral technique – hands-on soft-tissue manipulation
- Pediatric and Pregnancy Specific adjustments – hands on but specifically designed for certain times of life
- Webster Technique – pelvis alignment for turning breech babies